Trends in COVID-19 Infection and Deaths Observed Across 63,000 Nursing Home Residents
April 2020 data from the CarePort Transitions of Care Hub
What are the characteristics, underlying conditions, and trends of nursing home residents infected with COVID-19? While much has been written on COVID-19 outbreaks in nursing homes, limited information exists at the resident-level. Descriptions exist in the hospitalized population, but there is a lack of trending on the impact of age, sex, and underlying conditions on COVID-19 in the nursing home population. CMS is expected to release information on COVID-19 cases and deaths at nursing homes at the end of May. While preliminary, we hope that this report, which focuses on nursing home resident-level trends, complements the facility-level reporting to be released next week.
This report is based off of 63,000 long-term care residents in nursing homes in April 2020. 10,000 residents were COVID-19 positive, of which 755 died in April 2020. Residents were identified based on their diagnosis as captured in the electronic health record.
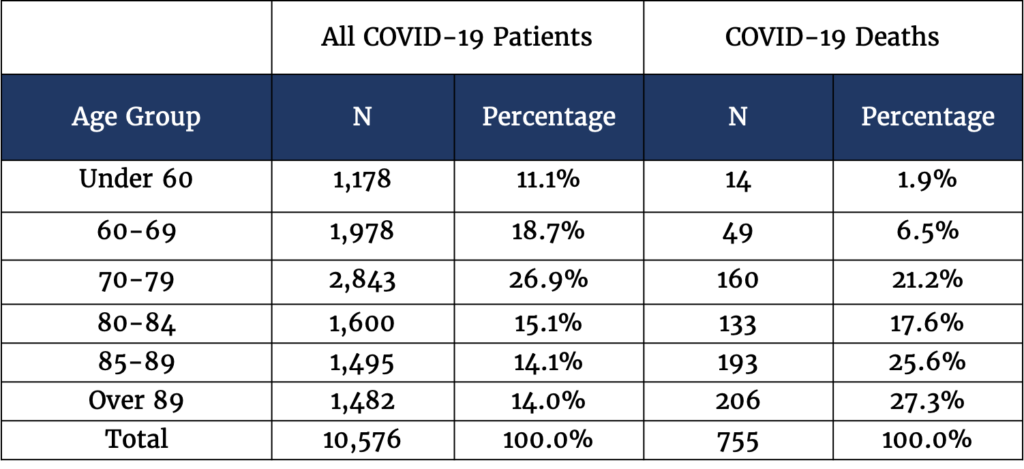
Increasing age is associated with COVID-19 deaths in the nursing home population, with the most vulnerability observed among the residents aged 85 and older
As consistent with prior reports, increasing age is associated with increasing risk of COVID-19 mortality. This is especially pronounced in the population of residents who are 85 years and older. For example, while residents 85 years and older constituted less than a third of total COVID-19 cases in nursing homes, this group made up over 50% of COVID-19 deaths.
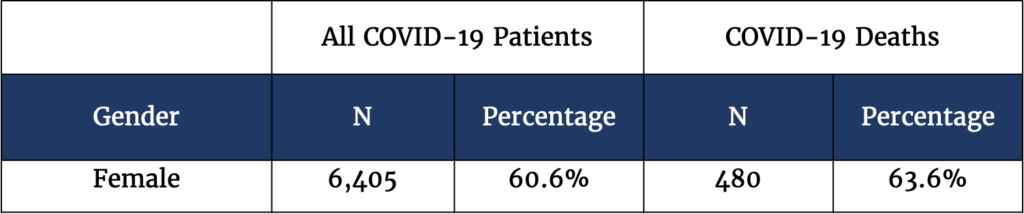
Female residents represent 60% of COVID-19 deaths
In the nursing home population, female residents make up 60% of COVID-19 patients and deaths. Nationally females constitute 44% of COVID-19 deaths (according to CDC data as of May 9, 2020), the skew towards female in the nursing home is reflective of overall demographics of nursing homes. And in states such as Massachusetts, where nursing homes residents account for 60% of COVID-19 deaths, more women than men have died of COVID-19.
Dementia is correlated with increased risk of COVID-19 death in the nursing home population
In the nursing home population, dementia appears to be associated with a 1.7x risk of death, even after adjusting for age. It is important to adjust for age as increased age may be associated with increase prevalence of dementia. While residents with dementia accounted for 52% of COVID-19 cases, they constituted 72% of all COVID-19 deaths in the nursing home.
Prior reports in the general population have focused on underlying conditions such as diabetes, COPD, heart failure, hypertension, obesity and kidney disease. In these findings, which are preliminary, only the impact of dementia could be observed. Importantly, our finding is consistent with other models that predict mortality in nursing homes, where dementia is a common underlying condition. One possible explanation is that dementia patients, who have impaired cognition and communication, may be diagnosed with COVID-19 at later stages. Furthermore, while dementia is often thought of as a memory problem by the general public, advanced dementia, which may be more prevalent in nursing homes, affects multiple organ systems and therefore may be less severe when facing an illness such as COVID-19. Further study is warranted to explain this association.
This is not to say that underlying conditions such as diabetes do not have an impact on the nursing home population, only that the effect did not achieve statistically significance in our current analysis. This may be due to data limitations as detailed below.
Data limitations:
- Data only includes confirmed COVID-19 cases; suspected cases are not included.
- Data may be subject to lead-time bias; diagnosis date of COVID-19 was not accounted for.
- Nationally according to CDC data between February 1 and May 16, 2020, just over 15,000 of COVID-19 deaths occurred in the nursing home or long-term care facility setting. We analyzed 755 COVID-19 deaths in April 2020, which represent approximately 5% of COVID-19 nursing home deaths in the US to date.
- COVID-19 deaths may have occurred in the hospital for residents who were transferred to the hospital. These are not accounted for in COVID-19 deaths here, as is consistent with CDC data, which defines location of death as “where the death was pronounced or the physical location where death occurred.”
A first look at nursing home resident trends with more to come
This report represents a preliminary view of patient trends associated with COVID-19 cases and deaths in nursing homes. As we continue to dive into the data, we expect to present more detailed descriptions, including further characterizations of the impact of common underlying conditions in the nursing home population, incorporation of outcomes of nursing home residents transferred to hospitals, and reporting on facility-level effects on COVID-19 outcomes.