In our recent blog post, we summarized the first virtual installment of our Care Coordination Summit series, “COVID-19 in Detroit,” sharing how a health system, post-acute provider and payer – Henry Ford Health System, Advantage Living Centers and Health Alliance Plan – pivoted quickly, increased communication, and collaborated across the continuum and community to successfully coordinate care during the COVID-19 surge in Detroit.
Sue Craft, Vice President, Inpatient Case Management and Post-Acute Care Services, and Gloria Rey, Post-Acute Care Director, Department of Population Health, spoke on behalf of Henry Ford Health System to discuss the challenges faced and lessons learned when managing COVID-19 patient transitions in Detroit during the surge. Below, we explore Henry Ford’s experience – including the referral and discharge process complexities when COVID-19 first reached their hospitals, the technology updates made in partnership with CarePort to streamline patient transitions, and increased collaboration and transparency with post-acute partners to ensure optimal patient care.
Referral and Discharge Process Complexities
Henry Ford saw its first COVID-19-positive patient in one of their hospitals on March 13 – and within the month there were 15,312 COVID-19-positive cases in Detroit. Between March and July, there were more than 4,000 COVID-19-positive hospitalizations at Henry Ford. These hospitalizations had a longer length of stay than they had ever seen before, and 24% of these admissions required the ICU, while 16% required ventilator support.
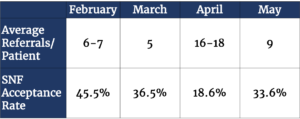
As is evident from the table below, COVID-19 brought about significant referral and discharge challenges for Henry Ford, and it became increasingly difficult for case managers and discharge planners to find SNF placement for COVID-19-positive patients. Though there was a slow decline in the health system’s SNF acceptance rate in March, the number of SNFs denying new patients skyrocketed in April. Prior to the pandemic, Henry Ford sent an average of 7,500 referrals per month. In April, however, the number of referrals sent by Henry Ford nearly tripled, as SNF placement for patients became exceedingly challenging. At the peak of the COVID-19 surge in Detroit – with 350 COVID-19-positive patients in Henry Ford ICUs and nearly 300 of their COVID-19-positive patients requiring ventilator support – Henry Ford hospitals nearly became COVID-19-dedicated hospitals because of the number of positive patients. Unable to discharge patients from the hospital, Henry Ford was forced to create holding areas for patient overflows as it struggled to manage bed capacity.
Technology Updates to Alleviate Challenges
Working with CarePort, Henry Ford quickly implemented technology changes to improve patient care and streamline patient transitions from the acute to post-acute setting. These small but impactful updates included:
- Adding a patient’s COVID-19 status to the first page of the referral to facilitate easier referrals for post-acute providers. SNFs were immediately aware of a patient’s positive, pending or negative COVID-19 status.
- Within CarePort Guide, Henry Ford could view and sort SNFs based on their ability and willingness to accept COVID-19-positive patients – as well as their isolation bed availability – which improved SNF acceptance rates.
- Using CarePort Connect and CarePort Insight, Henry Ford could share pending COVID-19 test results with providers post-hospital discharge. COVID-19 testing was initially very slow, and patients needed to be discharged from hospitals in the meantime. By sharing COVID-19 results with SNFs post-discharge, the post-acute facility could move patients from isolation to a more appropriate location based on their status.
- Twice-daily COVID-19 status reports indicated which patients were COVID-19-positive or had pending results, which facilitated dialysis centers in the scheduling necessary appointments, and placing patients in the appropriate chairs to ensure their safety.
Regarding these technology changes, Gloria Rey said: “The CarePort team that we worked with were absolutely fantastic and we got these changes up and running sometimes within a couple of days… the survey took a large amount of IT uplift but they had it up and running within the week.”
Working with Post-Acute Partners to Optimize Patient Care
During this time, Henry Ford also worked collaboratively and increased communication with its partners across the continuum through daily meetings, as well as weekly SNF corporate leadership meetings, during which the health system’s SNF partners joined together and worked collaboratively to identify barriers to optimal patient care. This increased communication enabled Henry Ford to better understand what was going on in the community, in order to assist SNFs in addressing their most critical challenges – which included PPE and staffing shortages, and a lack of access to testing. For example, to help its partners in a time of need, Henry Ford donated its surplus PPE – 70,000 N-95 masks, 800,000 pairs of gloves and innumerable gowns and face shields – to post-acute facilities.
Lessons Learned through the COVID-19 Surge
During the COVID-19 surge in Detroit, Henry Ford learned the critical importance of communication and transparency. Their daily morning huddles with cross-continuum partners, as well as SNF corporate leadership meetings, were immeasurably helpful in understanding SNF challenges. Product changes within CarePort also ensured that Henry Ford and its post-acute partners could successfully coordinate cross-continuum patient care.
To streamline care transitions, Henry Ford has also learned the importance of understanding each individual facility’s testing requirements. This will be an area of focus moving forward; Henry Ford is currently working with the CarePort team to implement this functionality – which will simplify processes and save time for both case management teams and SNFs – into CarePort Guide.
Watch the full-length recording of the live case study, and stay tuned for upcoming blog posts where we’ll detail the experiences of Advantage Living Centers and HAP during Detroit’s COVID-19 surge.